Heart disease is the leading cause of death in the United States.
Since researchers first established the link between diet, cholesterol, and heart disease in the 1950s, heart disease risk has been assessed in part based on a patient’s cholesterol levels, which can be routinely measured through blood tests in the doctor’s office.
However, accumulating evidence over the past two decades has demonstrated that a biomarker called C-reactive protein, which indicates the presence of low-grade inflammation, is a better predictor of heart disease risk than cholesterol.
you may like
What is C-reactive protein?
C-reactive protein is produced by the liver in response to infections, tissue damage, chronic inflammatory conditions due to conditions such as autoimmune diseases, and metabolic disorders such as obesity and diabetes. Essentially, it is a marker of inflammation in the body, and thus the activation of the immune system.
C-reactive protein can be easily measured with an in-office blood test. Low levels of C-reactive protein (less than 1 milligram per deciliter) means there is minimal inflammation in the body, which protects against heart disease. An increase in C-reactive protein levels of more than 3 milligrams per deciliter means increased levels of inflammation and therefore increased risk of heart disease. Approximately 52% of Americans have elevated levels of C-reactive protein in their blood.
Research shows that C-reactive protein is a better predictive marker for heart attack and stroke than “bad” cholesterol (short for low-density lipoprotein) and another commonly measured genetically inherited biomarker called lipoprotein(a). One study found that C-reactive protein can predict heart disease just as much as blood pressure.
Why is inflammation important in heart disease?
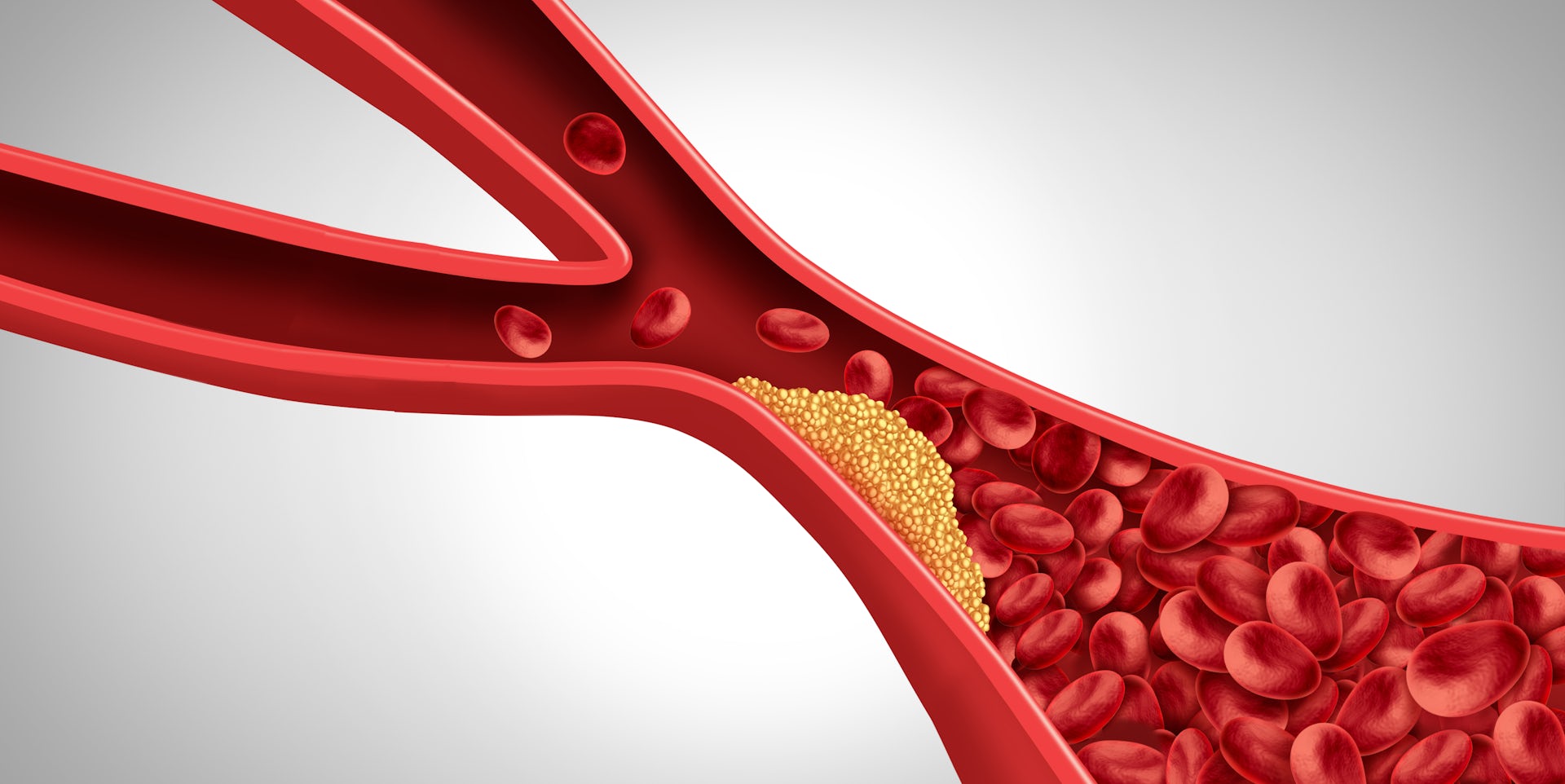
Inflammation plays a key role in every step of the development and buildup of fatty plaques in the arteries, leading to a condition called atherosclerosis that can lead to heart attacks and strokes.
The moment a blood vessel is damaged, whether by high blood sugar or cigarette smoke, immune cells immediately invade the area. These immune cells then engulf cholesterol particles that are normally floating in the bloodstream, forming fatty plaques that reside on the walls of blood vessels.
This process continues for decades until one day the immune mediators rupture the cap surrounding the plaque. This causes blood clots to form, which restricts blood flow and deprives surrounding tissue of oxygen, ultimately leading to a heart attack or stroke.
you may like
So cholesterol is only part of the story. In fact, it is the immune system that facilitates each step of the process that causes heart disease.
Can diet affect C-reactive protein levels?
Lifestyle can have a significant impact on the amount of C-reactive protein produced by the liver.
Many foods and nutrients have been shown to reduce C-reactive protein levels, including dietary fiber from foods such as beans, vegetables, nuts, seeds, berries, olive oil, green tea, chia seeds, and flaxseed.
Weight loss and exercise can also reduce C-reactive protein levels.

Does cholesterol still affect heart disease risk?
Cholesterol may not be the most important predictor of heart disease risk, but it’s still relevant.
But it’s not just the amount of cholesterol, or more specifically the amount of bad cholesterol, or LDL cholesterol, that matters. Two people with the same cholesterol levels do not necessarily have the same risk of heart disease. This is because the risk is determined by the number of particles packed with bad cholesterol, rather than the total mass of bad cholesterol floating around. The more particles there are, the higher the risk.
That’s why a blood test known as apolipoprotein B, which measures the number of cholesterol particles, is better at predicting heart disease risk than measuring the total amount of bad cholesterol.
Like cholesterol and C-reactive protein, apolipoprotein B is influenced by lifestyle factors such as exercise, weight loss, and diet. Nutrients such as fiber, nuts, and omega-3 fatty acids are associated with a decrease in the number of cholesterol particles, and increased sugar intake is associated with an increase in the number of cholesterol particles.
Additionally, lipoprotein(a), a protein found in the walls surrounding cholesterol particles, is another marker that can predict heart disease more accurately than cholesterol levels. This is because the presence of lipoprotein (a) makes cholesterol particles sticky, so to speak, making them easier to get trapped in atherosclerotic plaques.
However, unlike other risk factors, lipoprotein (a) levels are purely genetic, so they are not influenced by lifestyle and only need to be measured once in a lifetime.
What is the best way to prevent heart disease?
After all, heart disease is the product of many risk factors and their interaction over a lifetime.
Therefore, preventing heart disease is much more complex than simply eating a cholesterol-free diet, as once thought.
Knowing your LDL cholesterol levels, along with your C-reactive protein, apolipoprotein B, and lipoprotein (a) levels, provides a comprehensive picture of your risk and will hopefully help motivate your long-term commitment to the basics of heart disease prevention. These include eating well, exercising consistently, getting enough sleep, managing stress productively, maintaining a healthy weight, and quitting smoking if applicable.
This edited article is republished from The Conversation under a Creative Commons license. Read the original article.
Source link