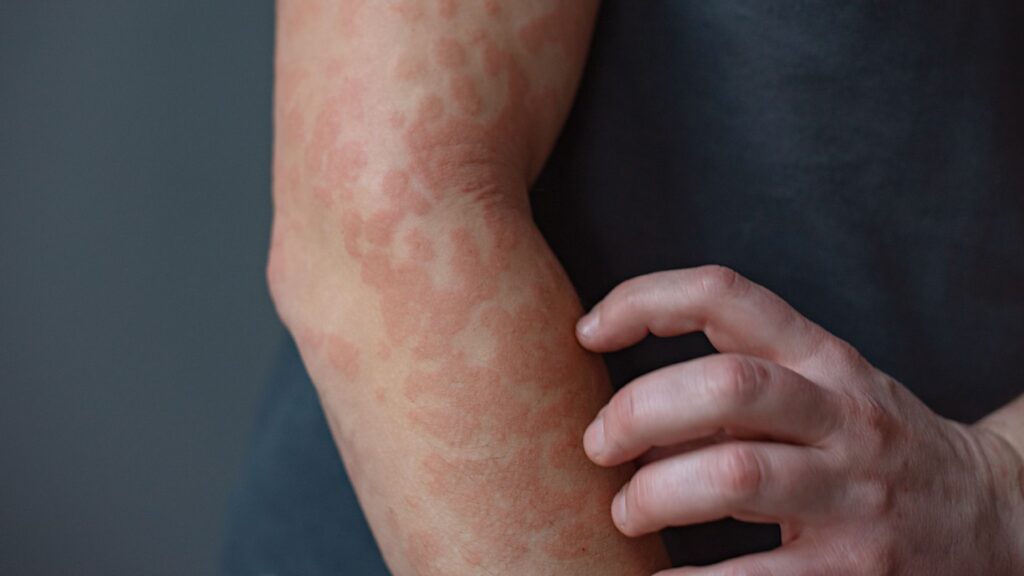
Keratin proteins, which form our skin, hair and nails, can confuse the immune system and cause diseases such as psoriasis and eczema when mutated, new research suggests.
In a new study published Wednesday (April 8) in the journal Science Translational Medicine, researchers have identified a mutant form of the keratin protein that can disrupt processes that normally help skin cells manage inflammation. This breakdown may help explain how inflammatory skin diseases occur.
you may like
The role of keratin in skin inflammation
The researchers focused on PC because this genetic disease is known to be caused by mutations in the KRT16 gene, which carries instructions for keratin-16.
In PC, these mutations disrupt the network of filaments that help skin cells in high-friction areas of the body, such as the soles of the feet, resist mechanical stress. As a result, activities such as walking or running destroy skin cells and cause inflammation, forming painful calluses and blisters.
The skin of people without PC increases the production of keratin-16 when faced with stress factors such as inflammation.
“Keratin is like the steel cables and steel beams of cells,” Wendy Borag, a professor in Augusta University’s Department of Physiology who was not involved in the study, told Live Science. “The tension necessary for the skin, [without it] It is easy to break or tear. When microorganisms invade, the immune system can react and cause inflammation. ”
And in people with chronic skin inflammation, the tissue continually produces large amounts of keratin16.
“If we can understand why these specific keratin proteins proliferate during inflammation and directly cause disease when mutated, we may be able to identify new ways to treat PC, psoriasis, and related conditions,” Cohen and Coulombe said.
What to read next
Therefore, Cohen, Coulombe, and colleagues aimed to elucidate the mechanism between keratin 16 and PC. They examined samples of thickened skin from PC patients and samples from laboratory mice with similar symptoms. They also disabled the KRT16 gene in a second group of mice to see what would happen if the gene no longer worked at all.
They found that when the keratin 16 gene is mutated or missing, skin inflammation spikes. According to Cohen and Coulombe, these results suggest that “K16 acts as a ‘brake’ on the signals normally produced by skin cells to recruit the immune system.”
These signals included type I interferons, a family of proteins that help control inflammation and coordinate immune responses to viruses and cancer.
The researchers found that type I interferon signaling was more active in both PC patients and mice than in asymptomatic people and mice. A similar increase was seen in mice lacking keratin 16, suggesting that in the absence of keratin 16, interferon activates a strong immune response and increases inflammation.
Conversely, the presence of keratin-16 modulated the activity of these interferons and reduced inflammation.
Historically, keratin 16 has been “best known as a structural protein,” Cohen and Coulombe said. Learning about this alternative function “completely changes the way we look at the skin’s defense system and the role keratin plays within it,” the researchers said.
Borag noted that the study was thorough and the results appeared convincing.
“This paper is even more impressive than I expected in terms of all the different techniques and approaches used to show that keratin-16 modulates interferon signaling in the skin,” she said. “When you use multiple different techniques and multiple different approaches and they all confirm the same thing, that’s a very powerful way to show that what you’re seeing is real.”
The study authors are optimistic that their findings could have a major impact on the treatment of skin diseases in the future. Indeed, in this study, we demonstrated that inhibitors of type I interferon were helpful in eliminating skin lesions in a PC mouse model.
“Understanding this newly discovered association creates an opportunity to examine type I interferon signaling as a new therapeutic target in PC,” the researchers said.
This article is for informational purposes only and does not provide medical advice.
Cohen, E., Xu, Y., Ghodke, S., Orosco, A., Wang, D., Johnson, CN, Steen, K., Sarkar, MK, Özlü, N., Tsoi, LC, Gudjonsson, JE, Marchal, L., Hovnanian, A., Parent, CA, and Coulombe, PA (2026). Keratin-16 inhibits type I interferon responses in differentiating keratinocytes in stressed and diseased skin. Science Translational Medicine, 18, eadx9123. 10.1126/scitranslmed.adx9123
Source link