A new study has found that contracting COVID-19 during pregnancy significantly increases the risk of pre-eclampsia due to blood pressure problems, but getting vaccinated can help prevent this serious pregnancy complication.
Studies consistently show that COVID-19 can worsen pregnancy outcomes. New research suggests that during the pandemic, pregnant women who contracted coronavirus infection had a 45% increased risk of preeclampsia compared to those who did not. Unvaccinated women had a 78% increased risk if they contracted the coronavirus.
you may like
If confirmed, these findings would represent a “groundbreaking advance” in understanding the potential link between pre-eclampsia and viruses, study co-lead author Dr Jose Villar, professor of perinatal medicine at the University of Oxford, told Live Science.
“Talisman effect”
Approximately 3% to 8% of pregnant people develop preeclampsia, usually during the second half of pregnancy or soon after giving birth. Preeclampsia is characterized by persistent high blood pressure and protein in the urine, which is often a sign of kidney damage. It can also cause blurred vision, vomiting, severe headaches, and sudden swelling of the face, hands, and feet.
Preeclampsia can lead to serious complications, including liver and kidney damage, strain on the heart, and obstruction of the placental blood supply. In some cases, the disease can progress to eclampsia, which can include swelling of the brain, seizures, and coma. Both preeclampsia and eclampsia can be life-threatening to mother and baby.
Scientists do not know exactly what causes preeclampsia. It is not entirely clear whether placental dysfunction causes preeclampsia or is a result of it, although some studies suggest that it is caused by abnormal growth of the placenta. That said, new evidence is emerging that viral infections, such as COVID-19, may play a role in causing changes in the immune system in some cases, leading to vascular dysfunction, a key process behind the symptoms of preeclampsia.
Bilal’s team speculated that a COVID-19 vaccine could help limit that risk by lowering the odds of contracting COVID-19 and severe disease. They also theorized that vaccination may strengthen the overall immune system, thereby protecting against other infections and blood vessel damage.
In the study, published February 18 in the journal eClinicalMedicine, researchers analyzed data from more than 6,500 women in 18 countries who became pregnant between 2020 and 2022. One-third of the participants were diagnosed with COVID-19 during pregnancy. Approximately 58% had not received a COVID-19 vaccination at the time of data collection. Of the remaining women, about 31% received a booster shot in addition to completing the first vaccination series.
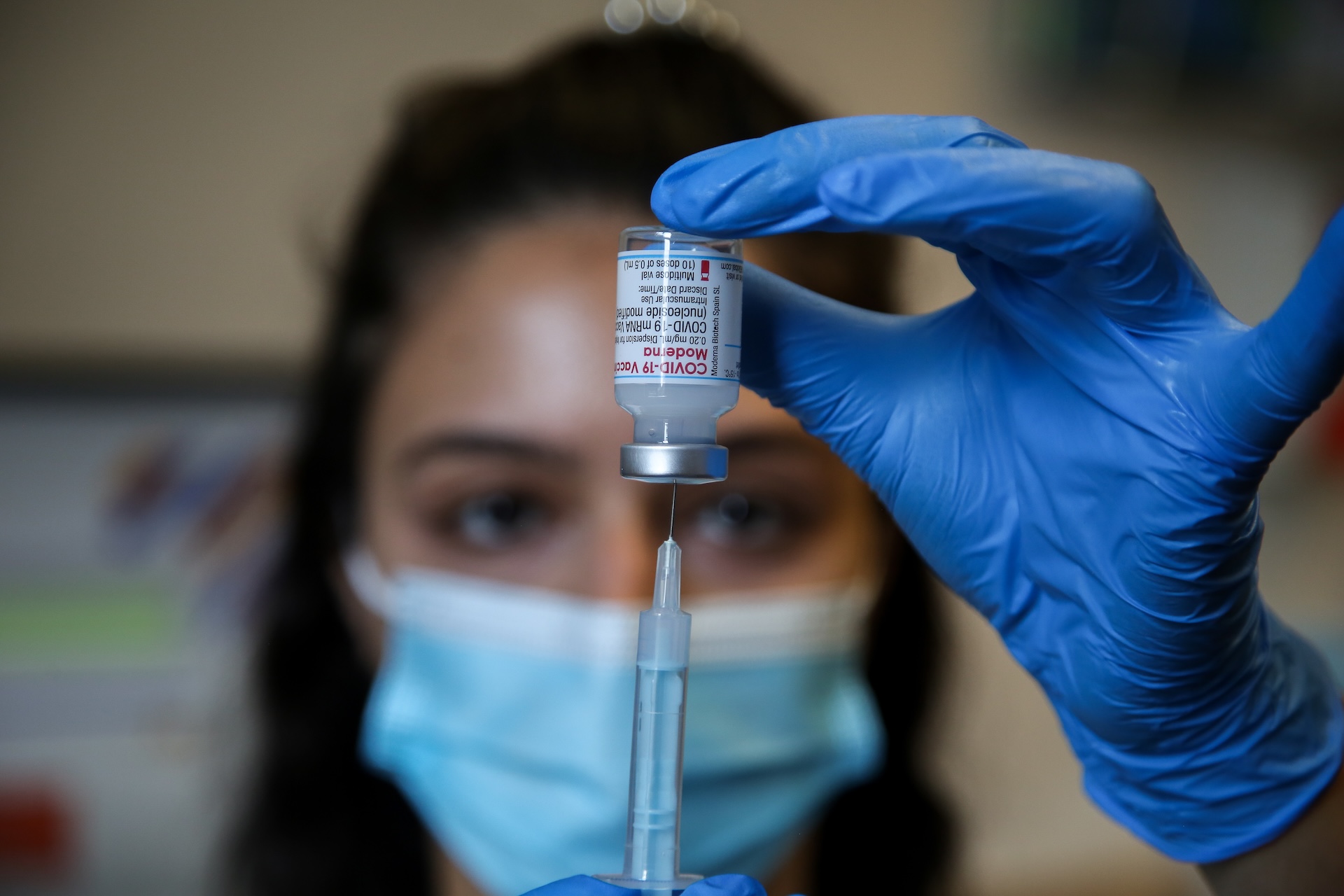
Researchers say vaccination appears to provide a “protective effect” against pre-eclampsia, and booster shots provide further protection. Notably, women who received the booster shot also had lower rates of poor overall pregnancy outcomes, measured as an index score that includes events such as preterm birth and intensive care unit admission, compared to women who did not receive the vaccine.
you may like
This is in line with research published in 2024, which found that women who received at least one dose of a COVID-19 vaccine were less likely to have a premature birth, stillbirth, or give birth to a baby that is small for gestational age than those who were not vaccinated.
“Vaccination is safe and can prevent some risks,” said Dr. Elena Raffetti, assistant professor at Sweden’s Karolinska Institute and lead author of the 2024 report. “There was no increased risk of preeclampsia at all among vaccinated women,” added Raffetti, who was not involved in the new study.
The authors of the latest study emphasized that their results support current vaccine guidelines. The American College of Obstetricians and Gynecologists recommends that pregnant women receive the latest coronavirus vaccine at the earliest opportunity, either while trying to conceive, during pregnancy, while breastfeeding, or during the postpartum period.
The new analysis has some limitations. For example, although the researchers tried to control for factors that could influence the results, such as the woman’s age, smoking history, and health issues associated with pre-eclampsia, such as a history of high blood pressure or diabetes, Professor Villar said there may be other differences between the vaccinated and unvaccinated groups that contribute to the risk.
The study authors said future research into the causes of preeclampsia should focus on how the immune system responds to both infections and vaccines, and why infections like COVID-19 appear to increase the risk of the condition.
Villar said much is still unknown about the causes of preeclampsia, and new insights could help researchers understand this “significant disease that affects mothers and fetuses.”
This article is for informational purposes only and does not provide medical advice.
Cavolet, P.I., et al. (2026). Covid-19 vaccination status and preeclampsia risk during pregnancy: the pandemic-era cohort of the INTERCOVID consortium. eClinicalMedicine, 103785. https://doi.org/10.1016/j.eclinm.2026.103785
Source link

