Patient: 20-year-old male living in China
Symptoms: Patient had a red cross tattoo on his neck, just below his voice box. But after three months, the ink disappeared.
Article continues below
you may like
The patient presented to the hospital approximately 5 months after the tattoo appointment. Antibiotics and topical steroids were prescribed, but the symptoms did not improve.
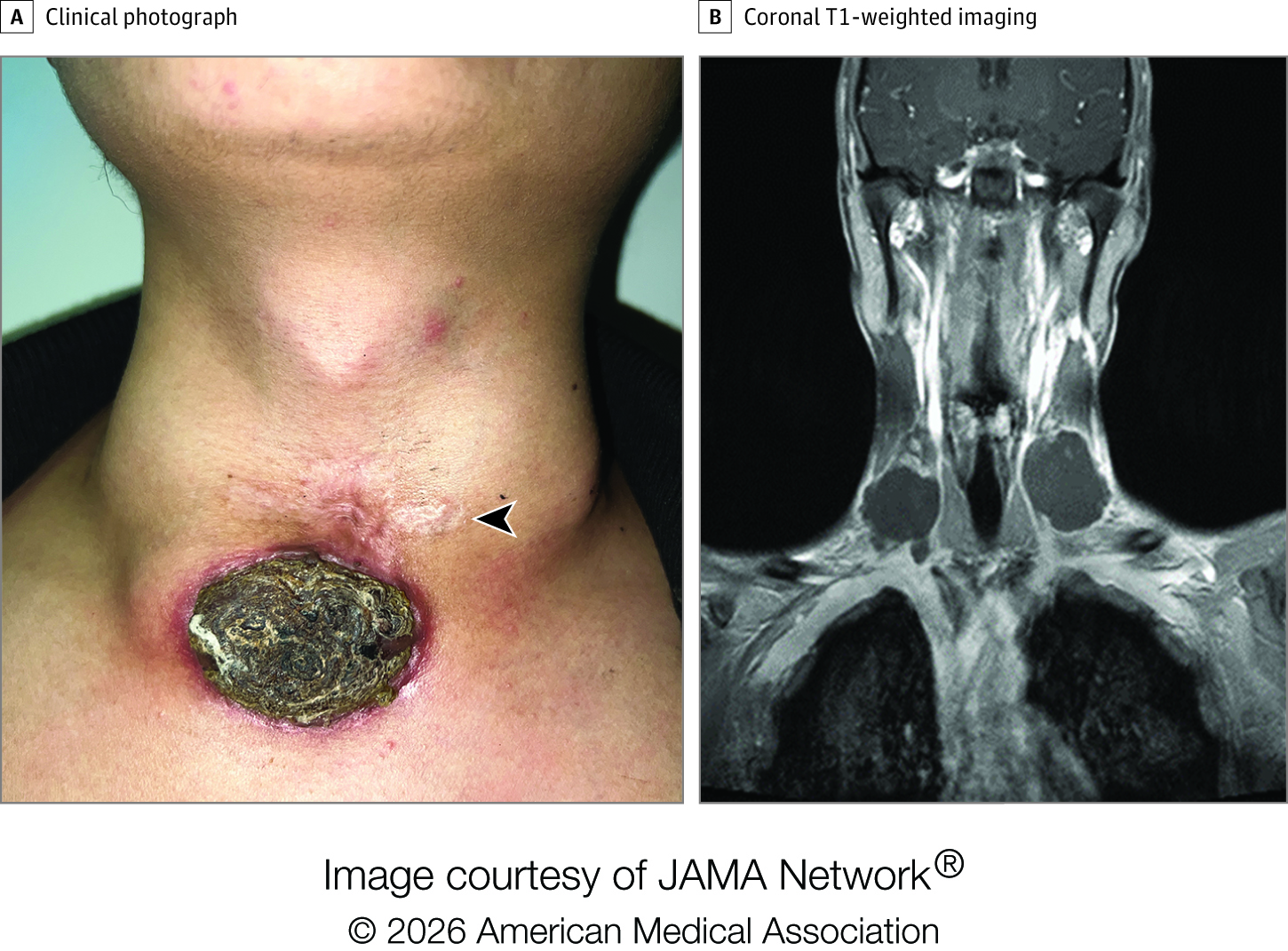
What happened next: Doctors physically examined the patient and found hard, swollen lymph nodes on either side of his neck, just below his jaw. They also examined a large necrotic ulcer in the center of the base of his neck and found that a scab-like mass had spread to deeper layers of the skin.
An MRI scan revealed that the lumps on each side of the man’s neck were approximately 4 x 3 centimeters, and the central mass beneath a large necrotic ulcer was 4.9 x 1.4 inches (4.9 x 3.5 centimeters). An enhanced CT scan revealed blood clots in the two jugular veins closest to the midline of the neck.
Doctors then used a thin needle to biopsy the necrotic ulcer, which revealed dead cells, immune cells and scar tissue. This did not indicate what caused the necrosis. However, the medical team became concerned about the scan results and the rate at which the man’s condition was progressing, so the patient was immediately sent to surgery, doctors wrote in the case report.
The research team removed the ulcer and mass and tied off the clotted jugular vein to prevent blood flow. The patient’s neck was then reconstructed using tissue from her thigh.
Diagnosis: The team performed immunohistochemistry on the biopsy sample, using antibodies to look for specific antigens, or substances that trigger an immune response. The results were negative for both Epstein-Barr virus, the bacteria that causes the mono-infection, and tuberculosis, but a type of benign tumor-forming cell was detected.
“Together, these findings supported the diagnosis of necrotizing granulomatous lymphadenitis,” the doctors wrote. “Granulomatous” refers to a condition in which clusters of immune cells form a wall around a persistent infection or foreign body.
What to read next
Necrotizing granulomatous lymphadenitis is an immune response to an injury to the body, in this case a man’s cross tattoo. The doctors also noted in the report that heavy metals such as mercury and cadmium, as well as red organic dyes found in tattoo pigments, can cause a delayed immune response. However, since no disappeared tattoo pigment was detected in the surgically removed lesions, their contents could not be directly examined.
Treatment: After surgery and a short course of hormone therapy, doctors reported that the man made a full recovery. (They did not say what kind of hormone treatment he received or why it was needed.)
What’s unique about this case: Tattoos can come with potential health risks, including allergic reactions and skin infections. In a study of 226 people who had reactions to tattoos, granulomatous reactions were relatively common, accounting for 48% of the inflammatory reactions reported.
Doctors noted that the man’s case was the second known case of necrosis reported after a tattoo. In other known cases, patients experienced lipoid necrosis, a rare inflammatory skin disease in which collagen in the skin breaks down, and early granuloma annulare, characterized by a raised, ring-shaped rash.
Doctors said the man’s necrotic ulcer was also unusual in that it was particularly aggressive and had spread deep into the skin.
Doctors suggested three potential causes of the man’s severe necrosis. First, the chronic inflammation and heightened immune response caused by the tattoo may have increased the risk of blood clotting. Alternatively, enlarged lymph nodes on the side of the neck may press on the jugular veins, slowing blood flow. A final possible explanation is that chronic inflammation has begun to erode the walls of the veins.
Overall, “this report expands the scope of tattoo-related pathology,” the doctors wrote in their report. However, given that this is the second known case, this is likely a very rare outcome.
For more interesting medical cases, check out our Diagnostic Dilemma archives.
This article is for informational purposes only and does not provide medical advice.
Source link