Research suggests that for a long time, poor gum health is poor and high risk of cardiovascular disease. Now, new trials suggest that treatment for severe periodontal disease may reduce major arterial stenosis over time in healthy individuals.
Perhaps by reducing inflammation, this routine oral hygiene procedure may be an unknown way to minimize vascular deficiency.
“When I first saw the data, I was very overwhelmed,” Dr. Marco Orlando, a clinical researcher at University of London, told Live Science.
Approximately 40% of US adults over the age of 30 suffer from a certain level of periodontal disease known as periodontitis. This is a chronic inflammatory condition in which progression leads to loss of teeth, loss of teeth and persistent bad breath. As the illness worsens, small pockets around the teeth that cannot be reached with a toothbrush or floss expand and fill with plaque and bacteria.
Currently, there is a wealth of research that increases the risk of periodontitis for a variety of health outcomes, including Alzheimer’s disease, colon cancer and rheumatoid arthritis. An important area with evidence for mounts is the association between severe gingival disease and cardiovascular disease, and previous studies have found that periodontal disease management is associated with improved vascular function.
You might like it
Now, a clinical trial published on August 19 in the European Journal of Hearts found that treatment for periodontitis slows the thickening of the two layers of the inner carotid artery on both sides of the neck to an otherwise healthy adult. The thickness of these arterial walls is an important marker of the risk of cardiovascular disease.
Related: Keratin extracted from sheep wool repairs teeth with breakthrough
By targeting inflammation rather than other arterial health factors like cholesterol, “the impact of what we are doing occurs without going through the classic risk pathway,” Orlando said.
To test whether treatment for periodontitis actually causes long-term thickening of the carotid artery, Orlando and his periodontists and cardiologists conducted a gold standard trial at a dental hospital in central London. Because the trial was randomized, participants were randomly placed in treatment groups or in comparison groups that were not receiving intensive gum treatment.
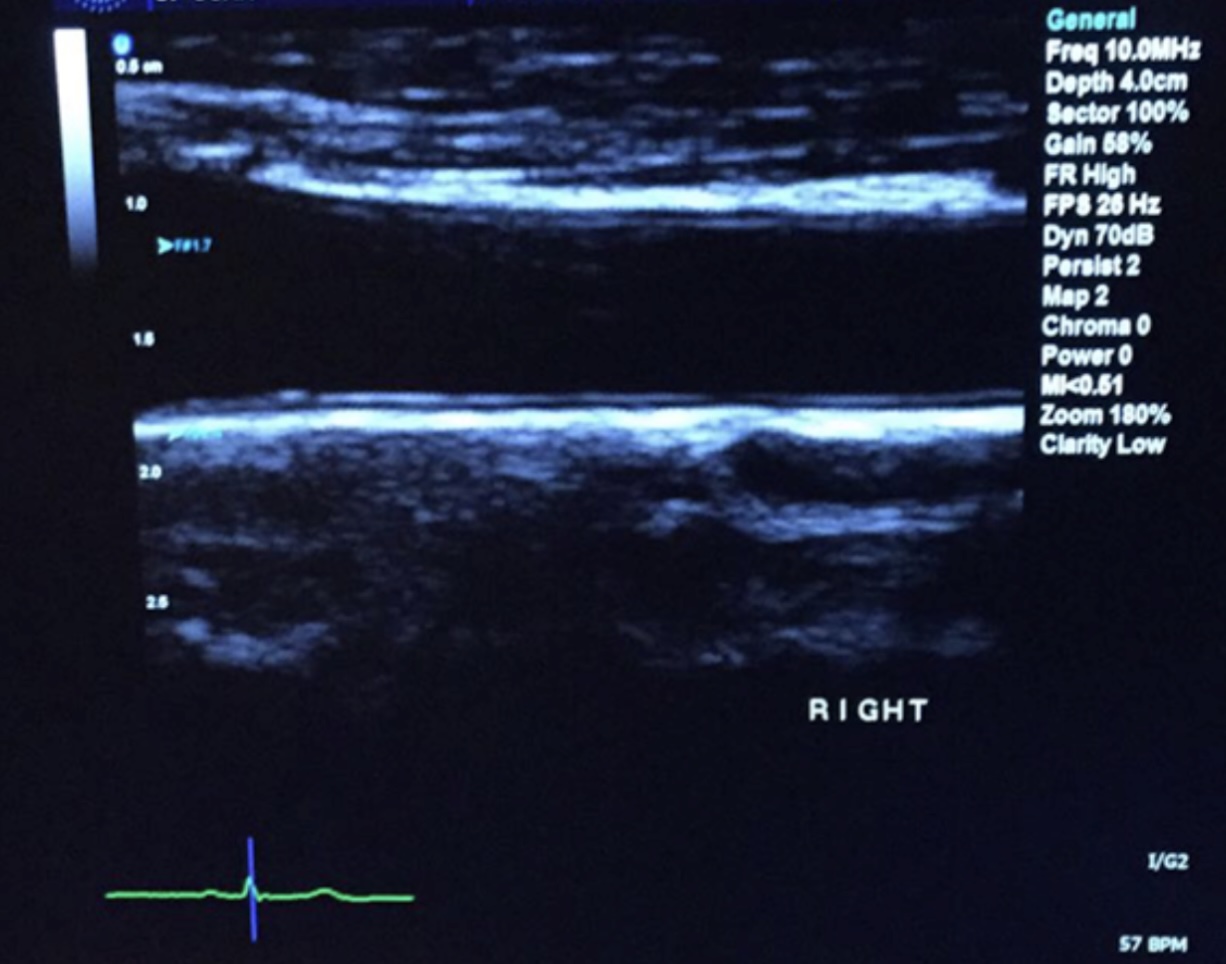
First, the researchers adopted ultrasound of 135 carotid arteries with severe periodontitis to establish a baseline level of thickness. They also measured how much arteries dilated when blood flow increased (a measure of blood vessel function) and took blood samples to identify markers of inflammatory and oxidative stress. All individuals were healthy other than having periodontal disease.
Participants were then randomly divided into either treatment or control groups. Care was taken to ensure that the participants were roughly divided between the two groups in terms of their periodontitis severity, smoking status, and family history of cardiovascular disease.
In the treatment group, patients received intensive periodontitis treatment. The entire mouth is thoroughly cleaned, and deeper under the gum line, removing plaque and tartar. The control group received simple scales and Poland, similar to regular dental cleanings that did not contain deep clean gums.
Participants were then followed for two years, each receiving further dental treatment on a regular basis during which time. The researchers also reevaluated the carotid artery at the 1 and 2 year marks, collected blood samples, and measured vascular function at five time points.
They found that the innermost medial neck thickness of the carotid artery was lower in those who received intensive care than in those in the control group. Co-authors of Francesco Daiute, a clinical research periodontologist at the University of London College, “compared to what was seen with some pharmacological agents in a similar population as lifestyle interventions,” the study co-authors, a clinical research researcher at the University of London, told Live Science in an email.
Treated patients have good vascular function and are known to contribute to arterial wall stenosis, due to lower levels of inflammatory and oxidative stress markers in the blood. This is a condition known as atherosclerosis.
While many factors promote atherosclerosis, “our results reinforce the view that untreated periodontitis is a modifiable risk factor for vascular aging and perhaps cardiovascular events,” D’Aiuto said.
However, an important limitation of the study is that it was carried out in only one location. So, Orlando said the findings could come down partially to the habits of location and people in the sample.
Another limitation is that Dr. Maurizio Tonetti, a clinical and research periodontologist at the University of Hong Kong who is not involved in the study, said that all participants in the study were healthy besides periodontitis. Therefore, these results should not be interpreted as evidence that when people with atherosclerosis are treating periodontal disease, he told Live Science.
Yet the findings bring these concepts [intensive gum disease] Interventions in conserving health,” Tonetti said.
“For years, dentists have focused on their teeth, forgetting the rest of their body, and doctors have been focusing on their bodies, forgetting that they have teeth,” he said. “They are really two separate worlds and they need to go back together for the benefit of the patients.”
This article is for informational purposes only and is not intended to provide medical advice.
Source link