On a hot Saturday in San Antonio more than 10 years ago, an 8-year-old boy was rushed to the hospital with several days of fever, headache, vomiting, and sensitivity to light. The child’s mother, who lived near the Texas-Mexico border, took her son to multiple clinics in Mexico, but his condition worsened. The child became unconscious and unresponsive to sound, light, and other stimuli.
Doctors put the child on a ventilator and began a frantic effort to figure out what was wrong. What they discover, swimming in the boy’s cerebrospinal fluid, is a creature that leaves little hope. It was Naegleria fowleri, widely known as the “brain-eating amoeba.”
you may like
However, Conrad recently read that a new drug option, miltefosine, has been approved as an experimental treatment for M. fowleri infections. He added it to the boy’s medication regimen, which already included other antibiotics and anti-inflammatory drugs.
“It’s the kitchen sink,” Conrad told LiveScience. “This is a bad disease. We just throw everything we can think of at them.”
The child’s prognosis was grim. He had been sick for five days before arriving in San Antonio, but most people infected with Fowleri infection die about five days after symptoms begin. According to the Centers for Disease Control and Prevention (CDC), from 1962 to 2022, there were 157 confirmed human cases in the United States, of which four survived.
Similar numbers are seen elsewhere in the world. Infections with this amoeba rarely make people sick, and survival is extremely rare. However, the few who survived may have recovered thanks to miltefosine, a new drug recently recommended for primary amoebic meningoencephalitis (PAM), a disease caused by an amoeba. New drugs may also emerge. The question is whether it can be delivered to patients before it causes any damage.
“The Bull in the Pottery Store”
According to the CDC, N. fowleri grows in warm freshwater above 80 degrees Fahrenheit (26.6 degrees Celsius), but can survive in colder temperatures. When water is forced into the nose, the amoeba infects people by pure chance, passing through a lacy bone called the lamina cribrosa and reaching the olfactory nerve, which acts as a highway to the brain.
Immunocompromised people are at higher risk, said Dr. Juan Fernando Ortiz, a neurology resident at Corewell Health in Grand Rapids, Michigan, who wrote a journal article on treating infectious diseases. According to the CDC, boys under 14 make up a disproportionate share of cases, likely because they are more likely than other groups to engage in activities that force water up their noses, such as jumping or diving. While most incidents involve natural bodies of water, few involve treated water such as splash pads. There have also been some cases of infections caused by using tap water in a neti pot to rinse sinuses.
The child Conrad and his colleagues were treating in August 2013 had typical symptoms of a tragic infection. He spent summers with his mother in an unofficial camp on the banks of the Rio Grande with no running water. People were bathing in the river, and children were enjoying playing in the shallows.
What to read next
Presumably, that’s where he encountered the amoeba, and Conrad and his team had to kill it before it wreaked such havoc that the child couldn’t survive.
The safest approach for those wondering whether they are at risk is to assume that Naegleria fowleri amoeba is present in all fresh water.
Dr. Julia Haston, a medical epidemiologist in the CDC’s Division of Waterborne Disease Prevention.
PAM causes death through extensive destruction of brain tissue. Although the amoeba itself carries out some of the destruction directly, earning it the nickname “brain-eater,” much of the brain damage is actually caused by the body’s aggressive immune response to invaders in its control systems, Conrad explained. Parasites that have evolved to live inside the body usually have ways to suppress the host’s immune response so they don’t lose their food ticket, Conrad said. However, N. fowleri does not require a host and therefore does not have these adaptations. “It’s the bull in the china shop,” said Conrad.
Fortunately, there are only zero to six cases of V. fowleri infections per year in the United States, and there is no evidence that infections are becoming more common, said Dr. Julia Haston, a medical epidemiologist in the CDC’s Division of Waterborne Disease Prevention. Most cases have occurred in Texas, Florida and other southern states, but in recent years there have been more cases in the northern United States than usual, perhaps because climate change is warming waterways to temperatures the amoeba prefers, and a 2021 study found an increase in cases from the Midwest as far north as Minnesota, Haston said.
“For people wondering whether they are at risk, the safest approach is to assume that Naegleria fowleri amoeba is present in all fresh water,” Haston said. “Lake, river, naturally occurring freshwater body.”

Hail Mary works
To combat the amoeba that was attacking the San Antonio patient’s brain, Conrad and his team turned to a then-novel treatment: miltefosine. The drug was originally an antibiotic used to treat leishmaniasis, a disease caused by a tropical parasite, and the CDC was distributing it to PAM cases because studies showed it was effective against P. fowleri. Miltefosine crosses the blood-brain barrier and is relatively well tolerated by patients, Ortiz said. This is important, he added, because many anti-parasitic drugs also damage human cells.
Doctors ordered the drug from the CDC. (It is now commercially available under the brand name Impavido.) It arrived 14 hours after the child was admitted to the hospital.
The child was alive.
But he wasn’t unscathed. When the boy was discharged from the hospital, he was able to breathe on his own, but couldn’t do much else. After months of rehabilitation, he regained some of his abilities, but his family still had to help with basic self-care, Conrad said.
But that same summer, a 13-year-old girl in Arkansas contracted an amoeba while swimming in an artificial pond. She received prompt treatment, including miltefosine, and recovered. After six months of rehabilitation, she had no residual neurological effects from this near-death, according to a 2015 case report describing her treatment.
She and the Texas boy are the first survivors of PAM in the United States since 1978. In 2016, a 16-year-old boy in Florida was infected with PAM and was given miltefosine. He also made a full recovery.
However, not all PAM patients treated with miltefosine survived. Even with new drugs, the fatality rate for PAM is over 97%, according to the CDC.
Every summer, several new cases of PAM emerge across the country, and doctors continually work to improve treatments. Conrad said he is increasingly looking at strategies such as lowering a patient’s body temperature to about 95°F (35°C), which some studies suggest may improve recovery from brain trauma.
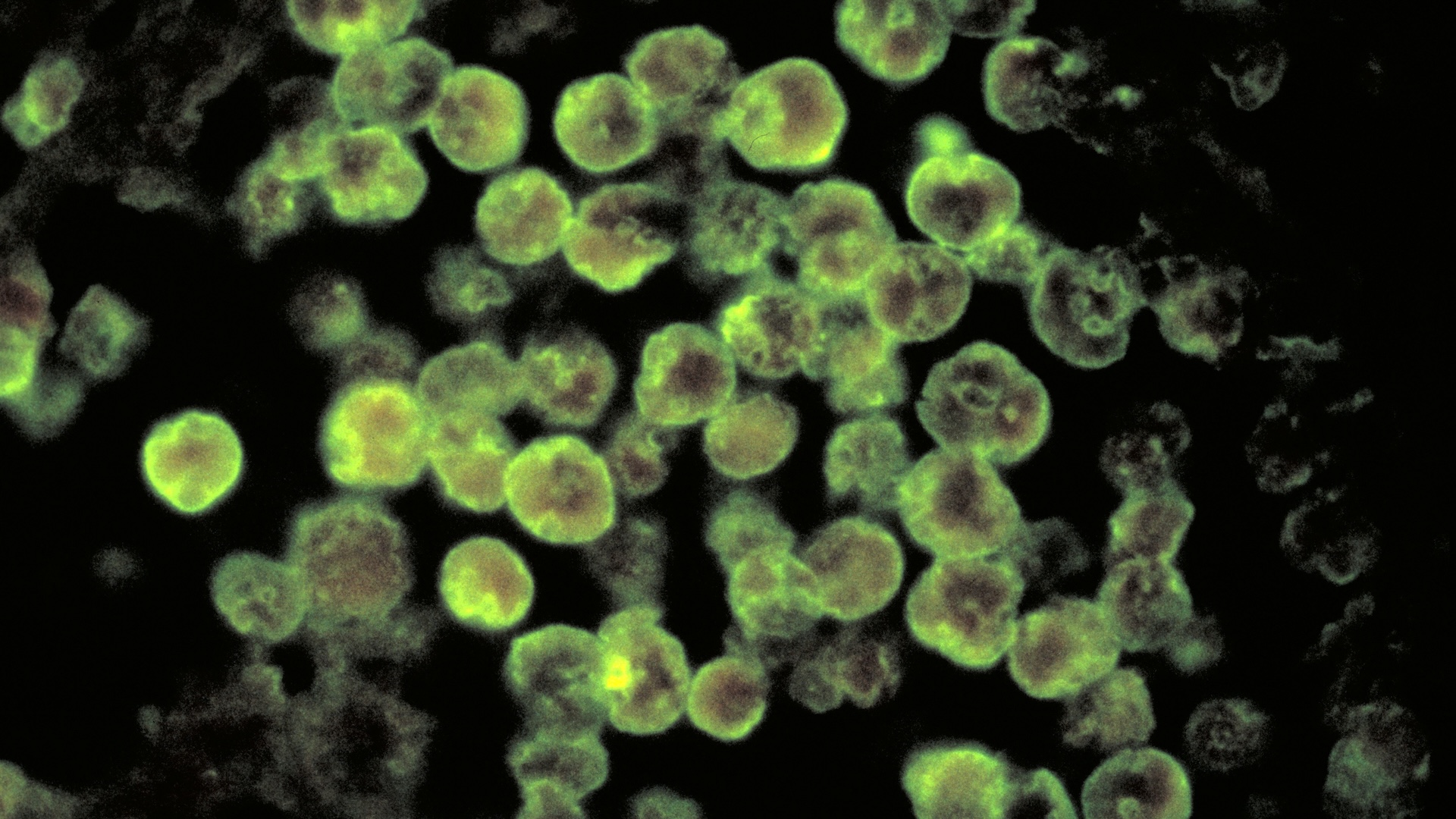
New medicines may also emerge. Jacob Lorenzo Morales, senior lecturer in parasitology and director of the Institute of Tropical Diseases and Public Health at the University of La Laguna in the Canary Islands, said miltefosine can cause toxic side effects on the kidneys and liver and is not available in developing countries.
So Lorenzo Morales and his team are looking for alternatives. One of the most promising is nitroxoline, an antibiotic used in Europe to treat urinary tract infections. Lorenzo Morales and his team reported in the journal Antibiotics in August 2023 that low concentrations of nitroxoline induced cell death of Clostridium fowleri in laboratory dishes without causing any toxic effects on host cells. The drug was also successfully used to treat one patient infected with another brain-eating amoeba, Balamusia mandrillaris.
They are currently conducting animal experiments and hope to present positive results at next year’s International Free Living Amoeba Conference, a biannual meeting of amoeba researchers. Nitroxoline is already widely available around the world and has already been approved for use, so large-scale clinical trials are not needed, Lorenzo Morales said. Your doctor can start using the drug off-label.
new replacement
Efforts are also being made to find new drugs that are effective against PAM. Some researchers are interested in developing an mRNA vaccine against V. fowleri infection, and a 2024 study published in the journal Scientific Reports used modeling of the amoeba’s surface features to suggest what such a vaccine might look like. (The authors of that study did not respond to Live Science’s interview requests.)
If it’s too late, it doesn’t matter which drug you use. Patients usually do not survive.
Julia Warochnik, Professor of Tropical Medicine at the Medical University of Vienna
Lorenzo Morales and his colleagues are also studying the effects of a pigment called erator, which is extracted from red algae. “We have isolated several important compounds from red algae that are highly active against a variety of free-living amoebas, including Naegleria, at even lower concentrations than current treatments,” he said.
However, researchers are currently conducting these tests in dishes in the lab. Moving tests to people will require funding from pharmaceutical companies. Lorenzo Morales said that could be difficult because companies don’t really think about the possibility of profiting from a “rare” disease like PAM. But PAM remains too often unrecognized, which may mean the potential market is larger than pharmaceutical executives realize, he said.
race against time
Perhaps the most pressing hope for patients today is simply recognizing the disease sooner. Julia Warochnik, a professor of tropical medicine at the Medical University of Vienna who studies amoebic diseases, says the window for saving PAM patients is short. “If it’s too late, it doesn’t matter which drug you use. Patients usually don’t survive,” she told Live Science.
The late start of treatment may be one reason why Conrad’s 8-year-old patient sustained such severe brain damage, while other young people treated at the same time made more complete recoveries.
Testing for amoeba is easy. Samples of fluid around the brain and spinal cord are taken to look for single-celled organisms swimming around. However, because PAM is similar to meningitis caused by more common viruses and bacteria, your doctor may not order the test in time. Families of children who have died from the disease are stepping up efforts to raise awareness, with the hope that this could lead to faster diagnosis and treatment. For example, the Jordan Smerski Amoeba Awareness Foundation, founded by the parents of an 11-year-old boy who died from PAM in 2014, hosts educational events for doctors and the public.
Lorenzo Morales said awareness is making a difference. “For the past four to five years, whenever we’ve been involved in a clinical case, the diagnosis has been made quickly,” he said. “That never happened before.”
Editor’s note: This article was originally published on July 26, 2024.
What do you know about the brain? Test your knowledge with our brain quiz.
Source link

